Here’s some food for thought: Would you compete in a CrossFit competition with only one week’s worth of training? Probably not.
In the same way, instead of deploying quick fixes to prevent illness like doubling up on Vitamin C, the immune system requires year-long training and strengthening in order to provide the best defenses against sickness.
When it comes to COVID-19, it’s important to understand what’s really happening to the immune system in order to deploy effective prevention and risk reduction strategies.
In our recent webinar, Dr. Leonard Calabrese from the Cleveland Clinic Center for Clinical Immunology joined Nicole Grasso, one of Bravo’s Wellness Strategists, to explain the immune response, risk factors related to COVID-19, strategies to reduce risk of exposure and severe illness from COVID-19 and how lifestyle impacts immune system functioning.
Read a summary of what Dr. Calabrese covered, and be sure to watch the recording for more details about the layers of our immune defense and protection from COVID-19.
How Does the Immune System React to COVID-19
While there are still unknowns about COVID-19, the current data shows that the majority of people who are infected (~90%) may be either asymptomatic or experience a moderate to severe flu-like illness lasting several weeks or more.
There other 10% will become extremely ill—many will end up hospitalized, about 5% will wind up in intensive care, and between 1-2% will die from the infection. But it’s not a coin flip to see which group one would fall into.
Here’s Dr. Calabrese describing how the body reacts to COVID-19:
“The people who do ‘well’ with COVID have two phases of illness. One when they get the infection, usually through a mucous membrane (mouth, nose, eyes) and that triggers the establishment of the infection, and it also triggers the immune system to send off these alarms and our defenses.
“Lucky people can defeat this within a matter of days, and it never actually even establishes itself. But most people, it goes on for another week or two. And that's when the immune system kind of pulls out the big guns starts making antibodies, just like in response to a vaccine. And we also have cells called T cells that attack the virus where it resides. When that's successful, that's the end of the game and we’re recovered.
“But in that 10%, something else happens. And it's you know, something that we have not talked about as a society. And that is the setting where the immune system is really set on fire. And what happens is that we can't get rid of the virus. The immune system keeps battling, but the problem is, is that in the heat of battle, there's now a lot of collateral damage to ourselves, to our lungs and our other organ systems. And so we die in this bonfire of what we call inflammation.
“There's a term that is used in clinical medicine and it's called cytokine storm. Kind of a graphic description. Cytokines are mediators of the immune system. They're proteins that cause all this inflammation, red, hot, swollen, tender, fever. Under ideal circumstances, never enter the cytokine storm. Unfortunately, we don't have a choice in that, and we know that there are risk factors for who winds up in stage three, the cytokine storm.”
As a reminder, the risk factors for severe illness are well-documented by the CDC: age and underlying medical conditions, including hypertension, diabetes and obesity.
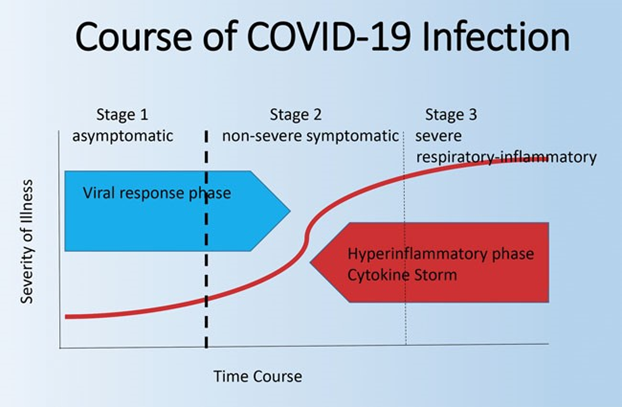
Image Source: Cleveland Clinic
Personal Behavior Can Reduce COVID-19 Risk
Maintaining a healthy immune system is based on several behavioral pillars but before talking about habits to adopt, we have to understand habits to avoid and what makes us vulnerable to infections.
“It doesn't do any good to try to de-stress or eat a healthy diet if we're a heavy smoker and we're not taking care of ourselves in all the ways that we know are healthy,” says Dr. Calabrese. Smoking, excesses in alcohol and drugs are a huge impediment to the immune system. But in the COVID era, Dr. Calabrese emphasizes, we must pay attention to hygiene.
In the same way that reducing chronic disease risk by eating healthy or practicing meditation is impeded by continuing to smoke, it still doesn’t make any difference to de-stress, get more sleep or exercise more if you’re not going to wash your hands and then touch your eyes, nose and mouth.
Dr. Calabrese’s main point of emphasis on hygiene and slowing the spread of COVID-19 is wearing a mask. He says, “What we're learning is that about 30 to 40% of people are either asymptomatic feeling healthy or pre-symptomatic. In other words, you may be healthy for a day or a week or 10 days, then they get this. So the reality is, is that as you walk down that street and you walk into your store and you look at that person next to you and they look pretty darn healthy, it's no guarantee that they don't have COVID-19 and spreading it readily.
“[Wearing a mask] is really about protecting others. I don't care if you're tested every day for this, you still have the opportunity to become infected. So when I see someone with a mask on, they're basically telling me, I care about you. And I care about those around me. It's an act of kindness. It's an act of humanity. And if we all wore masks and protected each other, because this does more to protect the other person than it does to protect you. This would stop this thing in its tracks.”
Adding Layers of Protection
Consider the “Swiss Cheese Model,” introduced in 1990 by James Reason. Safeguards are in place in any work setting to prevent risk – each safeguard is represented in this model as multiple layers of swiss cheese because every process, or safeguard, has holes. But under the right circumstances, the different layers of security can keep your workplace safe.
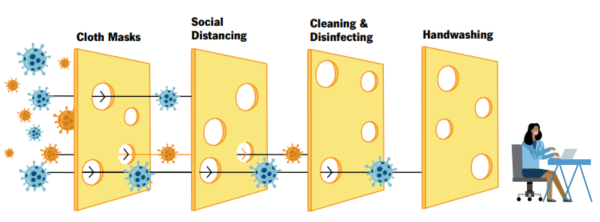
Image Source: Cleveland Clinic
Stay Tuned for Part Two: Evidence-Based Practices to Improve Immune Health
All that being said, there are proven ways to improve immune system functioning through personal behavior and healthy lifestyle choices. Can’t wait until next week? Watch the webinar recording for tips from Dr. Calabrese on the evidence-based practices.


